
Email : info@gghospital.in | Phone : +91 99622 29940
IMSI /PICSI
Home » IMSI /PICSI
Male infertility is on the rise due to men adopting drastic changes in lifestyle, in addition to added environmental insults and genetics, exactly in that order. Our lifestyle choices contribute to the bulk of cases. ICSI was a breakthrough in helping create biological offspring as opposed to the use of donor sperms but now a new entrant seems to be fine tuning this by a highly magnified selection process. Intra cytoplasmic morphologically selected sperm injection (IMSI) as it is popularly referred to have taken the technology to a higher level.
We need to look at a group of variables before we accurately select the cases that would need this procedure. According to literature survey this technique is of great benefit in cases of idiopathic infertility with repeated ART failures, oligoasthenozoospermia, previous miscarriages and cases which are subjected to PESA or TESE both of which are well known sperm retrieval techniques for azoospermia. A comprehensive work up of the male would include complete physical examination, personal history, occupation with related hazards, sexual history and last but most importantly the semen analysis.
Pointers from any of these could predict the prognosis of the conception cycle. We also need to remember that there is still no “absolute” definition for the normalcy of semen analysis. There are norms but at no point can a normal analysis be taken as a highly fertile sample as opposed to a subnormal one. When it comes to the moderately or severely oligo-astheno- zoospermic male, we need to ascertain if functionally normal sperms are present and if they are, how are we going to select them?
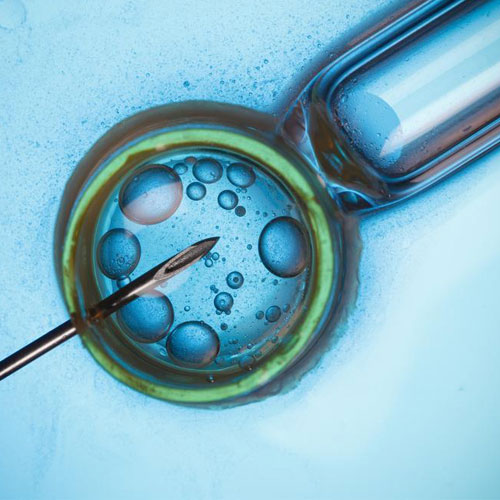
It is well known that sperms from an infertile male can be prone to chromosomal variations and also carry a possibility of passing on genetic defects to the offspring. In such a scenario, there is also the need to create a biological offspring ensuring at the same time that genetic defects are minimized. Time tested interventions are the PGD, amniocentesis and karyotype analysis. More recently FISH analysis of sperms comes in handy to rule out chromosomal abnormalities in poor semen samples and in men with translocations or other variations. But what if we could influence selection of a normal sperm by changing the optics of our already existent ICSI set up from a magnification of 200x to 6000x?
The selection process is called the motile sperm organellar morphology examination (MSOME) technique which assesses nuclei shape and configuration as well as homogeneity of nuclear chromatin mass. There are lab requirements to be fulfilled such as use of special optics, glass bottomed dish as well as density gradient preparation of sperms but given the almost doubled pregnancy rates in comparison to conventional ICSI this is one fast forward progression in ART !
Make your appointment now
